Retitled and cross-posted from the June 30, 2015 posting (Testing times: the future of animal alternatives) on the International Innovation blog (a CORDIS-listed project dissemination partner for FP7 and H2020 projects).
Maryse de la Giroday explains how emerging innovations can provide much-needed alternatives to animal testing. She also shares highlights of the 9th World Congress on Alternatives to Animal Testing.
‘Guinea pigging’ is the practice of testing drugs that have passed in vitro and in vivo tests on healthy humans in a Phase I clinical trial. In fact, healthy humans can make quite a bit of money as guinea pigs. The practice is sufficiently well-entrenched that there is a magazine, Guinea Pig Zero, devoted to professionals. While most participants anticipate some unpleasant side effects, guinea pigging can sometimes be a dangerous ‘profession’.
HARMFUL TO HEALTH
One infamous incident highlighting the dangers of guinea pigging occurred in 2006 at Northwick Park Hospital outside London. Volunteers were offered £2,000 to participate in a Phase I clinical trial to test a prospective treatment – a monoclonal antibody designed for rheumatoid arthritis and multiple sclerosis. The drug, called TGN1412, caused catastrophic systemic organ failure in participants. All six individuals receiving the drug required hospital treatment. One participant reportedly underwent amputation of fingers and toes. Another reacted with symptoms comparable to John Merrick, the Elephant Man.
The root of the disaster lay in subtle immune system differences between humans and cynomolgus monkeys – the model animal tested prior to the clinical trial. The drug was designed for the CD28 receptor on T cells. The monkeys’ receptors closely resemble those found in humans. However, unlike these monkeys, humans have other immune cells that carry CD28. The trial participants received a starting dosage that was 0.2 per cent of what the monkeys received in their final tests, but failure to take these additional receptors into account meant a dosage that was supposed to occupy 10 per cent of the available CD28 receptors instead occupied 90 per cent. After the event, a Russian inventor purchased the commercial rights to the drug and renamed it TAB08. It has been further developed by Russian company, TheraMAB, and TAB08 is reportedly in Phase II clinical trials.
HUMAN-ON-A-CHIP AND ORGANOID PROJECTS
While animal testing has been a powerful and useful tool for determining safe usage for pharmaceuticals and other types of chemicals, it is also a cruel and imperfect practice. Moreover, it typically only predicts 30-60 per cent of human responses to new drugs. Nanotechnology and other emerging innovations present possibilities for reducing, and in some cases eliminating, the use of animal models.
People for the Ethical Treatment of Animals (PETA), still better known for its publicity stunts, maintains a webpage outlining a number of alternatives including in silico testing (computer modelling), and, perhaps most interestingly, human-on-a-chip and organoid (tissue engineering) projects.
Organ-on-a-chip projects use stem cells to create human tissues that replicate the functions of human organs. Discussions about human-on-a-chip activities – a phrase used to describe 10 interlinked organ chips – were a highlight of the 9th World Congress on Alternatives to Animal Testing held in Prague, Czech Republic, last year. One project highlighted at the event was a joint US National Institutes of Health (NIH), US Food and Drug Administration (FDA) and US Defense Advanced Research Projects Agency (DARPA) project led by Dan Tagle that claimed it would develop functioning human-on-a-chip by 2017. However, he and his team were surprisingly close-mouthed and provided few details making it difficult to assess how close they are to achieving their goal.
By contrast, Uwe Marx – Leader of the ‘Multi-Organ-Chip’ programme in the Institute of Biotechnology at the Technical University of Berlin and Scientific Founder of TissUse, a human-on-a-chip start-up company – claims to have sold two-organ chips. He also claims to have successfully developed a four-organ chip and that he is on his way to building a human-on-a-chip. Though these chips remain to be seen, if they are, they will integrate microfluidics, cultured cells and materials patterned at the nanoscale to mimic various organs, and will allow chemical testing in an environment that somewhat mirrors a human.
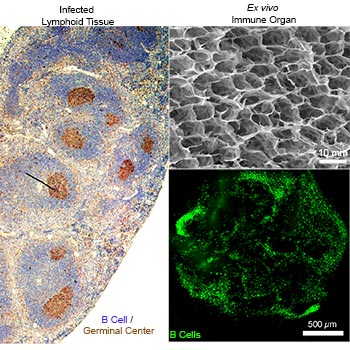
Another interesting alternative for animal testing is organoids – a feature in regenerative medicine that can function as test sites. Engineers based at Cornell University recently published a paper on their functional, synthetic immune organ. Inspired by the lymph node, the organoid is comprised of gelatin-based biomaterials, which are reinforced with silicate nanoparticles (to keep the tissue from melting when reaching body temperature) and seeded with cells allowing it to mimic the anatomical microenvironment of a lymphatic node. It behaves like its inspiration converting B cells to germinal centres which activate, mature and mutate antibody genes when the body is under attack. The engineers claim to be able to control the immune response and to outperform 2D cultures with their 3D organoid. If the results are reproducible, the organoid could be used to develop new therapeutics.
Maryse de la Giroday is a science communications consultant and writer.
Full disclosure: Maryse de la Giroday received transportation and accommodation for the 9th World Congress on Alternatives to Animal Testing from SEURAT-1, a European Union project, making scientific inquiries to facilitate the transition to animal testing alternatives, where possible.
ETA July 1, 2015: I would like to acknowledge more sources for the information in this article,
Sources:
The guinea pigging term, the ‘professional aspect, the Northwick Park story, and the Guinea Pig Zero magazine can be found in Carl Elliot’s excellent 2006 story titled ‘Guinea-Pigging’ for New Yorker magazine.
http://www.newyorker.com/magazine/2008/01/07/guinea-pigging
Information about the drug used in the Northwick Park Hospital disaster, the sale of the rights to a Russian inventor, and the June 2015 date for the current Phase II clinical trials were found in this Wikipedia essay titled, TGN 1412.
http://en.wikipedia.org/wiki/TGN1412
Additional information about the renamed drug, TAB08 and its Phase II clinical trials was found on (a) a US government website for information on clinical trials, (b) in a Dec. 2014 (?) TheraMAB advertisement in a Nature group magazine and a Jan. 2014 press release,
https://www.clinicaltrials.gov/ct2/show/NCT01990157?term=TAB08_RA01&rank=1
http://www.theramab.ru/TheraMAB_NAture.pdf
http://theramab.ru/en/news/phase_II
An April 2015 article (Experimental drug that injured UK volunteers resumes in human trials) by Owen Dyer for the British Medical Journal also mentioned the 2015 TheraMab Phase II clinical trials and provided information about the information about Macaque (cynomolgus) monkey tests.
http://www.bmj.com.proxy.lib.sfu.ca/content/350/bmj.h1831
BMJ 2015; 350 doi: http://dx.doi.org.proxy.lib.sfu.ca/10.1136/bmj.h1831 (Published 02 April 2015) Cite this as: BMJ 2015;350:h1831
A 2009 study by Christopher Horvath and Mark Milton somewhat contradicts the Dyer article’s contention that a species Macaque monkey was used as an animal model. (As the Dyer article is more recent and the Horvath/Milton analysis is more complex covering TGN 1412 in the context of other MAB drugs and their precursor tests along with specific TGN 1412 tests, I opted for the simple description.)
The TeGenero Incident [another name for the Northwick Park Accident] and the Duff Report Conclusions: A Series of Unfortunate Events or an Avoidable Event? by Christopher J. Horvath and Mark N. Milton. Published online before print February 24, 2009, doi: 10.1177/0192623309332986 Toxicol Pathol April 2009 vol. 37 no. 3 372-383
http://tpx.sagepub.com/content/37/3/372.full
Philippa Roxbuy’s May 24, 2013 BBC news online article provided confirmation and an additional detail or two about the Northwick Park Hospital accident. It notes that other models, in addition to animal models, are being developed.
http://www.bbc.com/news/health-22556736
Anne Ju’s excellent June 10,2015 news release about the Cornell University organoid (synthetic immune organ) project was very helpful.
http://www.news.cornell.edu/stories/2015/06/engineers-synthetic-immune-organ-produces-antibodies
There will also be a magazine article in International Innovation, which will differ somewhat from the blog posting, due to editorial style and other requirements.
ETA July 22, 2015: I now have a link to the magazine article.